The Animal Hospital, located in Westhampton, is a full-service veterinary hospital providing wellness, medical, and referrals to specialty practices.

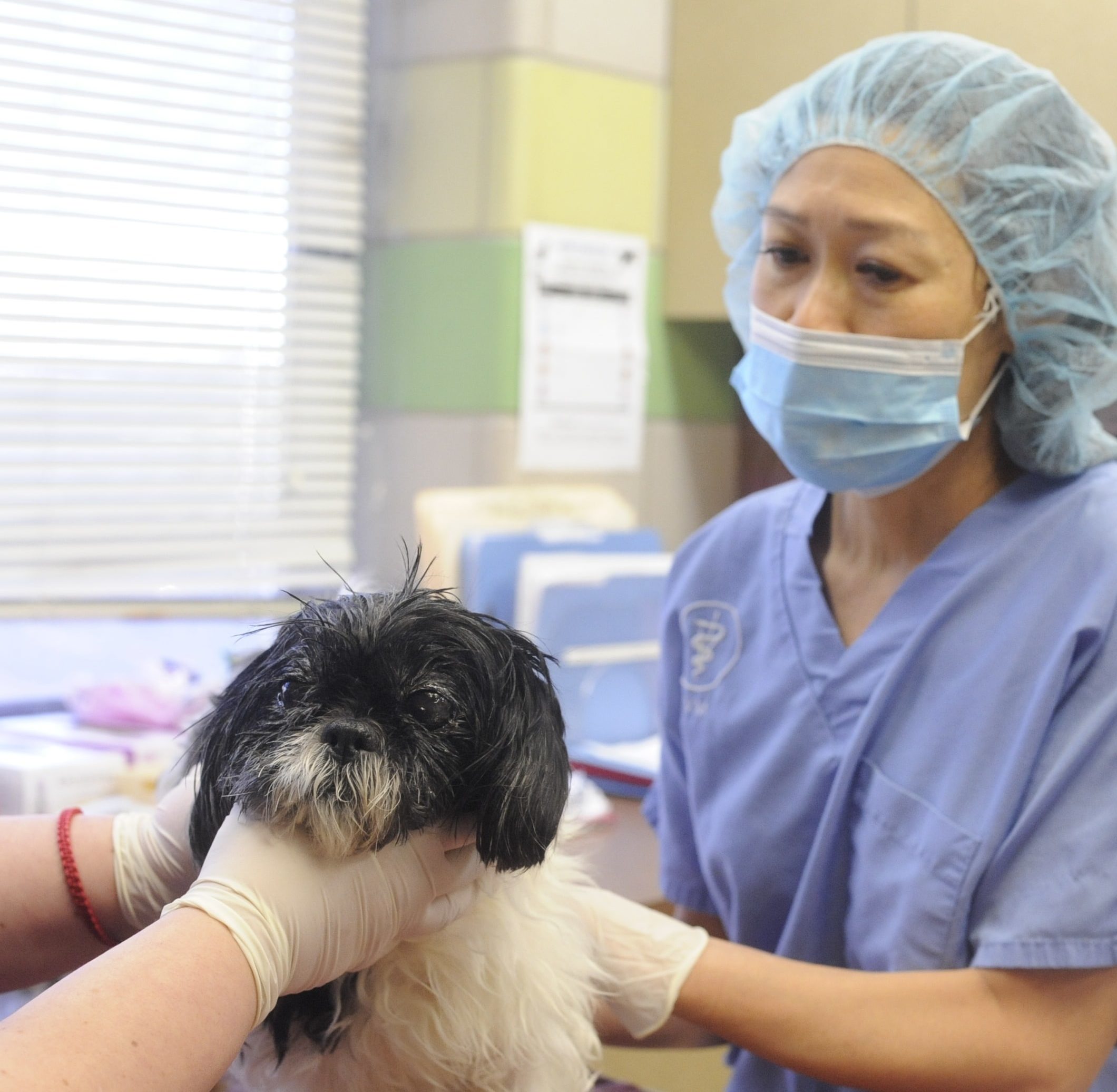
Services
- Wellness care: vaccinations and parasite control for cats and dogs
- Medical services: lab work including blood and urine tests, imaging services including radiographs and outpatient ultrasounds.
Meet Our Team
Medical Staff
The staff at the Animal Hospital at Bideawee, led by Dr. Melissa Young, are dedicated animal lovers that are committed to serving pets and the people that love them. The Animal Hospital at Bideawee provides access to highly-trained veterinary professionals that have experience in a variety of disciplines to care for any of your pet’s medical needs. The medical team at the Animal Hospital collaborates with pet parents to address current medical conditions and preventative health care.
Dr. Melissa Young, DVM
 Dr. Melissa Young has been a veterinarian at Bideawee since June 2012. She currently holds the position of Veterinary Medical Supervisor and oversees all medical decisions at Bideawee’s Westhampton hospital.
Dr. Melissa Young has been a veterinarian at Bideawee since June 2012. She currently holds the position of Veterinary Medical Supervisor and oversees all medical decisions at Bideawee’s Westhampton hospital.
A native of Nebraska, Dr. Young received her DVM from Kansas State University College of Veterinary Medicine. She also holds a Bachelor’s degree in Animal Science from Kansas State. Dr. Young has been engaged in small animal practice since graduating. She has divided her time between private practice in the mid-west and non-profit work around the globe. The non-profit work has taken her to places such as Senegal West Africa, Micronesia, and Easter Island.
Dr. Young enjoys cooking, gardening, and traveling when she is not working and loves her 2 Bideawee kitties Tocho and Chiquita.
Jennifer Midgett, LVT
Elizabeth Miller, Veterinary Assistant
Reception Staff
Roseann Sanzotta, Office Coordinator/Client Care Supervisor
Ashley Paduano, Client Care Coordinator
Contact Us
The Animal Hospital at Bideawee
118 Old Country Road
Westhampton, NY 11977
[email protected]
[email protected]
phone: 631-325-0280
fax: 631-288-0594
The Animal Hospital is by appointment only and is open 9am – 5pm, Tuesday, Wednesday, Thursday and Saturday.
